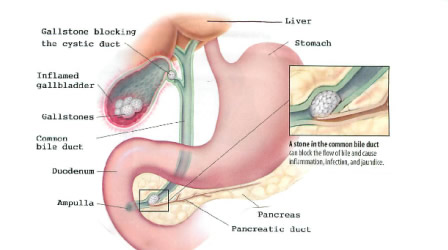
Gallbladder disease is a very common problem. Most often, symptoms are caused by gallstones in the gallbladder. To treat this, you will likely need to have your gallbladder surgically removed, which eliminates pain and future attacks.
Gallbladder problems can cause painful attacks, often after meals. Common symptoms include:
- Severe pain or aching in the upper abdomen. The pain may come and go or it can remain constant.
- A dull ache beneath the ribs or breastbone.
- Back pain or pain in the right shoulder blade.
- Nausea, upset stomach, heartburn, or vomiting.
Surgery will be done in the hospital. Follow the advice of your doctor on how to prepare for surgery. Tell your doctor about any medications (prescription or non-prescription) you are on (including supplements or herbs). Your doctor will instruct you as to whether you should stop any of these medications prior to surgery. Your doctor will advise you to stop taking aspirin, ibuprofen, and/or naproxen. If you are taking Coumadin, warfarin, or Plavix, your doctor will advise you when to stop taking this medication(s) and when to restart the medication(s). A family member or friend will need to give you a ride home after surgery. Do not eat or drink anything after midnight the night before your surgery. This includes water and coffee.
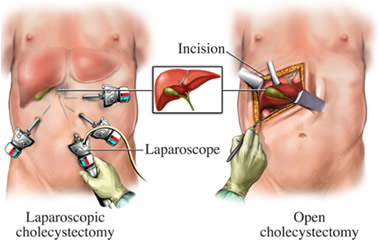
During surgery, your doctor will make a few small incisions in your abdomen. These are called port sites. The laparoscope is then inserted through one of these incisions. Using video images from the laparoscope, other surgical instruments are carefully guided to the gallbladder. Once the gallbladder is removed, the small incisions are closed with staples. The entire procedure usually lasts only 1 hour.
Your doctor may switch from a laparoscopic approach to an open approach. This is done when your doctor feels it is safer to remove the gallbladder through a larger incision. An open surgery means a longer hospital stay and recovery period from the surgery.
Gallbladder surgery is safe, but it does have certain risks: Bleeding, infection, injury to the common bile duct or nearby organs, blood clots in the legs, prolonged diarrhea, or bile leaks.
You can often leave the hospital the same day as your surgery. Make sure your surgery is a success by taking an active role in your recovery. You will likely feel tired. You may have some bruising around the incision sites. You may also have some abdominal cramping after a few days. This is normal and should go away in time. To help recovery, follow your doctor’s instructions. Remove your dressing as instructed by your doctor. Ask when it is okay to bathe again. Walk and move around as much as possible. Talk with your doctor about what to eat. It is normal to have pain during your recovery. Your doctor will prescribe pain medication for you to use at home. Take the medication as directed. Do not wait for the pain to get bad. Care for your incisions and manage your pain. Then begin easing back into your routine. Be sure to see your doctor for follow‑up care.
Getting Back to Normal
- Ask your doctor about driving and going back to work.
- Use pain relievers with acetaminophen to relieve discomfort.
- You can begin having sex again when you feel ready.
Eating Healthy Meals
- Once your gallbladder has been removed, you do not need to be on a special diet. It does take a few weeks though for your digestion to fully adjust. You may have indigestion, loose stools, or diarrhea. This is normal and should go away in time. To help you digestion, eat a balanced diet high in fiber. If any of these problems do not go away, tell your doctor.
Keeping Active
- To help your recovery, be as active as you can. Regular exercise improves blood circulation and is good for your whole body.
Follow-Up Care
- Keep your follow‑up appointments. Your doctor is able to check your progress. Discuss any concerns or questions you have.
If you notice any of the following during your recovery, call your doctor.
- Fever over 101° F.
- Chills.
- Sharp or increasing pain.
- Increasing redness, bleeding, or drainage from an incision.
- Vomiting or nausea that lasts more than 12 hours.
- Pain or swelling in your calves.
- Symptoms of jaundice.
- Prolonged diarrhea.